Louisiana Statistics
Drug Resistant TB Cases in Louisiana,1998-2018.pdf
Tuberculosis Control Program
Contact Us - Office of Public Health TB Control Staff Directory
Louisiana TB Morbidity Reports
Blood Assay for Tuberculosis - Decision to implement Blood Assay for Tuberculosis (BAMT)/ Interferon Gamma Release Assay (IGRA).
- Louisiana Adminstrative Code - Title 51: Public Health Sanitary Code
- Centers for Disease Control and Prevention, Division of Tuberculosis Elimination
- CDC Division of Tuberculosis Elimination - Educational Materials
- The American Lung Association of Louisiana
- Southeastern National Tuberculosis Center
dhh.louisiana.gov › Center for Community and Preventive Health
TB Update Contemporary Topics in MTB 2010
The Orleans Parish Triangle of TB
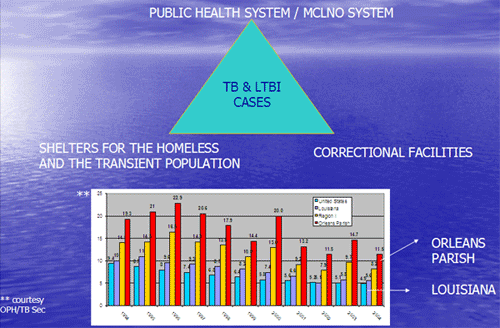
Click here to see larger version of chart
To Be Informed Newsletter
To Be Informed is a newsletter/brochure in Vietnamese and English based on frequently asked questions by audience and participants of the TEACH Program. It is distributed to community venues and primary care clinics.
Discussion Points
Tuberculosis Synopsis Update
- Definition : LTBI, “Chemoprophylaxis”
- Targeted tuberculosis testing in high risk/high prevalence groups and “precision treatment” options
- Three cut-off points for TST (tuberculin skin test) remain; However IGRA tests can substitute this test in certain circumstances
- US Public health Strength of recommendation ABC
- Quality of evidence I II III
- Duration of LTBI Rx: 6- 9 months
- Flexibility based on local public health considerations.
Recent Changes in Emphasis
- Criteria for PPD TST (tuberculin skin test) positivity, by risk stratification
- New definition of PPD TST (tuberculin skin test) converter: increase in 10 mm or more within a 2-year period.
- Clinical monitoring
- Lab monitoring in (a) HIV (b) pregnant (c) postpartum (d) Hx of liver disease
(e) Those who continue use of alcohol regularly. (f) Other medical conditions. For
cessation of Rx on the basis of LFTs recommended:
Rule of “FASTS” 5 times if asymptomatic; 3 times if symptomatic - Intermittent Rx must be DOPT
- Rifabutin in place of Rifampin in HIV patients where PI's are used
- In pregnant women with HIV or recent contact history or conversion, treatment should be started even in the first trimester.
- In other lower risk pregnant patients, Rx can be deferred till after delivery
- Options in INH resistant or PZA intolerant patients available
- Immune-competent contacts of MDRTB with LTB, PZA/ETM or PZA/QUIN for
6 months. - Immune-compromised contacts of MDRTB…………Rx for 12 months
Teaching Bullets
- Acid-fast
- Obligate aerobe: Involvement of spleen/heart?
- Intracellular
- Replication time 15-20 hours
- New Colonies generally do not appear after 6 weeks
- 99% Niacin-positive
- Flouroscient stain more sensitive than CF stain ( Overall: low sensitivity with 10000 (10 X4) bact/cc. Quantitatively: Rare= 3-9/slide; few =>10/slide; numerous 1/oil
- PCR: false positive
- DNA probe: rapid but expensive for ID
- Other AFB = Nocordia,Legionella Micadei
- 40-70 % of patients with MTB isolated on culture have positive smears
- Culture = egg based or agar based
- CXR: nodular= 10x2 -10x4; Cavitary=10x7-10x9
With treatment:
- Within 15 days: TB bacilli decrease 2 log i.e. 10x6 to 10x4
- Cough decreases in 40 % in 1 week and 65 % in 2 weeks
- Drug regimens that do not include INH do not render the patient non infectious as rapidly
- Operational implications regarding infectiousness should be modified depending upon living and working conditions.
- Under standard conditions and humidity, 60% survive 3 hours and 30 % survive 9 hours
Rate of TB:
- 15/1000 close contacts
- 3/1000 - close contacts
Control:
- BCG reduces the growth of organisms in macrophages
- In low incidence areas---endogeneous infection—Rx LTB
- In high incidence areas—exogeneous infection---TB control measures
PPD test:
- 48-72 hours -1 week. Plant Day 0 ; if not read in 7 days, replant 48-72 hours later
- Booster/2 step
| 0 | 2 weeks | result |
| - | - | - |
| - | + | + Booster Reaction, not conversion |
| + | + Positive |
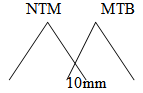
- Except in children, the size of the PPD TST (tuberculin skin test) reaction bears no relationship to the likelihood of active TB.
- BCG induced reactions are smaller and tend to wane more quickly than reactions caused by naturally occurring infections
- History of BCG generally ignored in the US
LTB: Treatment (Chemoprophylaxis)
- 80% reduction in incidence of active TB
- 50% less per year
- Overall 60% reduction
PULM TB - 35-80 % of patients have fever
- 11% have hyponatremia
- Single early morning specimens have higher yield and lower rate of contamination than pooled specimens. Increase in yield between 3-5 specimens is low
- Drug resistant mutants: ETH 10x4; INH/SM 10x6;RIF 10x8
- 8-16 % delinquent rates in 6 month DOT
- INH induced hepatitis: 10/1000 ( 0.1-0.3-3%)
- Retrobulbar neuritis with ETH: 15 % with 50mg/kg; 1-5% with 25mg/kg; <1% with 15mg/kg. Increased with renal dysfunction
- 50% of untreated TB patients die within 5 years
- 25% remain chronically ill with positive sputum cultures and infectious
- 25% resolve spontaneously
- Steroids in TB: Cachexia,shock,ARDS,Pericardial disease
- Lymphnode TB: Medical Rx after aspiration better outcome than surgical excision and Rx
- Pleural TB: 30 % have no evidence of pulm lesions on CXR
- Pl Fluid: 10 % eosinophils and 5 % mesothelial cells rules out TB
- POTTS: Two adjacent vertebrae with IV disk ( lower thoracic and upper lumbar)
- CSF : AFB smear 20% +, Culture 50-80%
- TB peritonitis: Active TB uncommon; 50 % have MTB culture positive
- GU TB: 50-70 % have old TB
- 50% of those with pericardial disease have pleural involvement
- Quantiferon TB Gold/TB Spot Test
- Gamma Interferon necessary for activation of microbicidal mechanism in macrophages
- Nitric Oxide: Microbicidal and bacteriostatic
- Murine macrophages which produce NO both inhibit growth and kill virulent human TB bacilli in vitro when activated by TNF alpha and gamma interferon
- Cytokines and lymphokines have the ability to organize granulomas and wall of infection, decrease bacillary load and restrict the mobility of infected macrophages and hence spread of infection
- In immune-deficiency individuals, decreased TNF causes lack of granuloma formation and hence unrestricted spread.
- Caseation necrosis and cavitation is due to killing of TB bacilli with cytokines and T lymphocytes
- MMWR - TIGRA TB Tests June 2010 Update
NTM/MOTT
Who Dat Mott 2011 PowerPoint Presentation
Of all Mycobacteria isolated in 41state labs
- 65% NTM
- 21% MAC
- 5% Mycobacterium kansasii (MyKS)
- MAC in HIV :serotype 4-8
- Rx of MAC in non immune compromised host: 50 % successful with 20 % relapse
Mycobacterium kansasii (MyKS)
- Colonization less frequent than MAC
- 53 % of those from whom MyKS isolated truly had invasive disease
- Same criteria of dx
- 35-40% have no significant lung disease
Rapid growers
- beaded gram positive rods on gram stain
- MyCh/Mfort: Sternal osteomyelitis, mediastinitis,pericarditis,vascular inv, aspiration pneumonitis
- MAC-PD Management Strategy & NTM Summary
For more information regarding NTM/MOTT, please click on the following link: Nontuberculosis Mycobacteria Info & Research
Contemporary Topics in MTB 2010 through the Wemore TB Clinic Tour
TB & HIV: Quadruple Jeopardy
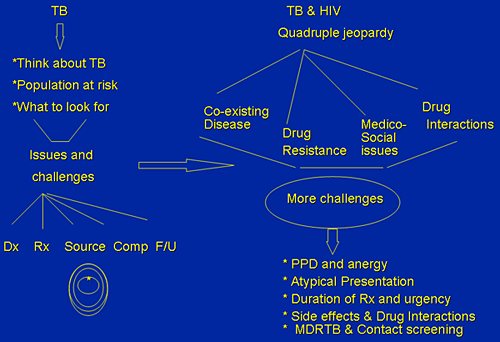
Atypical TB/NTM/MOTT : Background
Although most non-tuberculosis mycobacterium (NTM) are isolated from water, soil, and the environment and essentially may be ubiquitous, nevertheless, they may be hither to an under appreciated source of lung disease. NTM has been recognized as human pathogens as far back as 1950, and were prevalent in a distinct epidemiological setting in elderly white males, with an underlying chronic lung disease. Some forms of NTM's, specifically Mycobacterium avium-complex (MAC) are a frequent cause of opportunistic infection in immune compromised hosts and have been recognized more in the HIV population. However, NTM can also occur in immunosenescent individuals and even normal hosts, and not infrequently seen in geriatric population. Clinicians in the community have been aware of this increasing problem, but have been limited by the poor correlation that exists between bacteriological diagnosis of infection, and its clinical and radiological manifestation. This perpetuates an empiric and albeit challenging approach towards its treatment and management. Further, NTM infections in the form of MAC, M.Kansasii, M. Chelonei and M. Gordonoe to name a few, may not only co-exist with other infections, but require specific and different treatment regimes for variable durations. Since the advent of HIV in the 1980's, more attention has been paid to NTM infection. Recent reports of increasing incidents of this infection in middle-aged non-smoking females, with no underlying lung disease or no obvious immune deficiency state bring this problem to the attention of the public at large and the medical community in particular. National surveys in the early 80's indicated that about 33% of all mycobacterium isolates in clinical laboratories were due to NTM, and a later survey confirmed this observation. This data does not include patients with HIV and disseminated NTM disease, and neither does it factor the changing epidemiology of the infection as we see it today. In one suburban community survey in Virginia during the period of 1990-1992, twenty out of twenty-one cases of mycobacterium disease were due to NTM, and 80% of these were due to MAC. Being not a reportable disease, these are estimates based on indirect evidence. It is our observation also, that infection with NTM's represents a poorly recognized cause of lung infection in middle-aged and elderly patients in the community in Louisiana and the tri-state area.
Clinical information
X-ray findings in pulmonary tuberculosis with and without HIV infection has been described well. However, x-ray evidence of Atypical TB is non specific with pulmonary nodules and signs of scarring. All efforts to distinguish between colonization, persistent infection, and infection causing disease require a comprehensive correlation between clinical condition, bacteriological data, x-ray evidence, and progression of disease. This is not only a clinical challenge for the physician but a source of uncertainty for the patient and the family. The treatment protocols for such patients, once a need for treatment is determined, necessitates a long term multi-drug therapy plan, with substantial patient costs and increased morbidity both due to the disease, as well as, due to drug related side effects.
Because of the graphics involved, a high speed connection is recommended for the following material:
