Ventilation-Perfusion Relationships
I. Ventilation-perfusion relationships ( 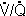 )
)
A. Concept: for optimal gas transfer to occur in the lung, ventilation and perfusion must be matched.
1. For the whole lung, alveolar ventilation and pulmonary blood flow are both about 5 L/min.
2. Therefore, for the whole lung 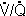 is about 0.8 - 1.2.
is about 0.8 - 1.2.
3. However, ventilation and perfusion must be matched on the alveolar-capillary level.
4. Local airway responses and hypoxic pulmonary vasoconstriction help match ventilation and perfusion.
B. Consequences of high and low 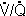 (Levitzky Fig. 5-1):
(Levitzky Fig. 5-1):
1. Normal
a. Inspired air entering alveoli:
PO2 = 150 mmHg; PCO2 = 0 mmHg
b. Mixed venous blood entering pulmonary capillaries:
PO2 = 40 mmHg; PCO2 = 45 mmHg
c. Result:
Alveolar PO2 = 100 mmHg;
Alveolar PCO2 = 40 mmHg
2. Low 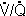
a. Extreme case - perfusion, but no ventilation (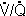 = 0): Complete airway obstruction or atelectasis leading to intrapulmonary shunt
= 0): Complete airway obstruction or atelectasis leading to intrapulmonary shunt
b. Result: PAO2 = 40 mmHg; PACO2 = 45 mmHg; no gas exchange
3. High 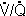
a. Extreme case - ventilation, but no perfusion (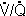 = infinity): no perfusion, leading to alveolar dead space
= infinity): no perfusion, leading to alveolar dead space
b. Result: PAO2 = 150 mmHg; PACO2 = 0 mmHg; no gas exchange
4. There is a continuum of 's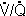 ranging from zero to infinity, resulting in a range of PO2's and PCO2's, as shown on the O2 - CO2 diagram (Levitzky Fig. 5-2). Low
ranging from zero to infinity, resulting in a range of PO2's and PCO2's, as shown on the O2 - CO2 diagram (Levitzky Fig. 5-2). Low 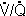 lower PO2's, higher PCO2's; high
lower PO2's, higher PCO2's; high 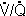 's higher PO2's, lower PCO2's.
's higher PO2's, lower PCO2's.
C. Tests of non-uniform gas distribution:
1. Single breath of O2 test. Monitor expired N2 concentration in "alveolar plateau" phase (Levitzky Fig.3-14). Steep plateau = non-uniform gas distribution.
2. N2 "washout" with O2. In a normal person alveolar N2 concentration is less than 2.5% after 7 minutes (Levitzky Figs. 5-3, 5-4).
3. Trapped Gas. Difference between FRC as determined by helium dilution and body plethysmograph techniques.
4. Single breath of 133Xe. Location of poorly ventilated areas by lung scan.
5. Technetium labelled aerosolized DTPA.
D. Tests for non-uniform pulmonary blood flow:
1. Pulmonary angiogram
2. Lung scan after injection of 131I or technetium labelled macroaggregates of albumin
3. Lung scan after intravenous 133Xe E. Tests of mismatched ventilation and perfusion:
1. Physiologic shunts:
a. Anatomic shunts - normally <2% of the cardiac output; bronchial veins, thebesian veins, and pleural veins.
b. Absolute intrapulmonary shunts
c. Shunt-like states - low 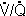
d. The shunt equation (Pulmonary venous admixture):
2. Physiologic Dead Space:
a. Anatomic Dead Space
b. Alveolar Dead Space
c. The Bohr Equation:
d. There is normally no arterial-alveolar CO2 difference. Arterial PCO2's greater than alveolar PCO2's (= end-tidal PCO2's, see Levitzky Fig. 3-9) indicate alveolar dead space (or possible diffusion block).
3. Alveolar-arterial O2 difference (Levitzky Table 5-2). Normally 5-20 mm Hg or age divided by 4 plus 4 mm Hg. Increased
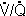 by mismatch, shunts, and diffusion block. Also increased by high FIO2's, low PO2's and shifts in oxyhemoglobin dissociation curve.
by mismatch, shunts, and diffusion block. Also increased by high FIO2's, low PO2's and shifts in oxyhemoglobin dissociation curve.
4. Alveolar plateau of the expired CO2 trace (Levitzky Fig. 3-9).
5. Lung scans after inspired and injected radioactive xenon or technetium.
6. Multiple Inert Gas Elimination Technique (Levitzky Fig. 5-5). 7.
II. Regional 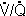 differences in the normal upright lung and their consequences (Levitzky Figs. 5-6,
5-7, 5-8).
differences in the normal upright lung and their consequences (Levitzky Figs. 5-6,
5-7, 5-8).
|
TOP |
BOTTOM |
|
|
1. Ventilation - less difference
|
more negative |
less negative |
|
2. Perfusion - more difference
|
lower |
greater |
|
3.
|
higher |
lower |
Copyright 2000 M. G. LEVITZKY
Last updated Friday, July 19, 2013 4:10 PM
LSUHSC is an equal opportunity educator and employer.
The statements found on this page are for informational purposes only. While every effort is made to ensure that this information is up-to-date and accurate, for official information please consult a printed University publication.
The views and opinions expressed in this page are strictly those of the page author. The contents of this page are not reviewed or approved by LSUHSC.
This page is maintained by webmaster-arc: mgiaim@lsuhsc.edu
